Introduction
The extraction of the mandibular third molar is the most frequent intervention in oral surgery and it is sometimes associated with less or more severe complications. Among these, the most dangerous is the damage to the inferior alveolar nerve.
In the last decades, thanks to the improved expertise in identifying risky cases and the refinement of surgical techniques, the prevalence of complications has been progressively reduced.
The present paper describes a rational approach to the surgical extraction of the mandibular third molar, in order to limit surgical complications.
As to the method, several factors contribute to the clinical success, just like:
- a correct pre-operative diagnosis;
- a rational choice of surgical instruments;
- a minimally invasive surgical technique.
The last two points are closely interdependent.
Pre-operative diagnosis
The diagnosis includes:
- study of indications and contraindications for surgery;
- risk and difficulty assessment;
- intervention planning.
The orthopantomogram (OPG) is the golden standard for pre-operative diagnosis.
From the OPG it is possible to evaluate:
- tooth position (angulation, depth, proximity to the neurovascular bundle);
- presence of risk factors for mandibular alveolar nerve damage, according to the criteria of Rood & Shehab (1990);
- diseases (caries, cysts etc.).
According to Rood & Shebab, the following risk indicators for damage of the mandibular alveolar nerve can be identified on OPG:
- root radiolucency;
- angled roots;
- interruption of the radiopaque lines that mark the alveolar canal;
- narrowing of the mandibular alveolar canal;
- radiolucent and bifid roots;
- narrowing of roots;
- deviation of the mandibular alveolar canal.
Nowadays, since the OPG does not allow to establish the bucco-lingual position of roots and neurovascular bundle, in particular cases it is possible to recur to 3D imaging, particularly to Cone Beam technology.
Clinical indications for 3D imaging are:
- signs of risk with complete overlapping of the roots to the alveolar canal;
- alveolar canal crossing the roots near to the bifurcation.
From an operative point of view, one more indication for 3D imaging is the necessity to understand on which side of the tooth the alveolar canal passes, in order to plan properly the bone resection and odontotomy.
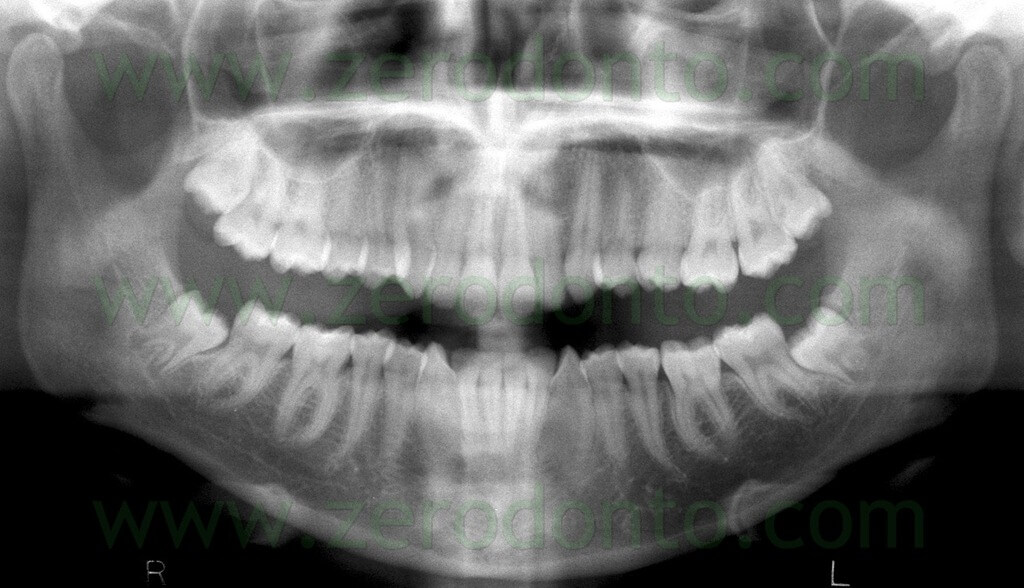
On this OPG, referring to 4.8, it is possible to notice the crossing between the alveolar canal and the tooth bifurcation and interruption of the radiopaque line that defines the alveolar canal (a risk factor according to Rood & Shehab, 1990).
On the computerized tomography (CT), the alveolar canal passes lingually to the roots.
Although 3D examinations greatly help to plan the intervention, to date no studies have been published demonstrating a better ability to prevent neurological damage.
Surgical instrumentation
The choice of the surgical instruments is not random but it is an integral part of the method.
In addition to standard surgery tools (scalpel, retractor, forceps for tissues, needle holder, rongeur), the tray for surgical extraction of impacted teeth includes some dedicated tools, such as spreaders, Friedman levers (both standards and reduced) and clamps for fragments.
Finally, a surgical handpiece with high speed burs designed for odontotomy completes the instrumentation.
Surgical technique
The operation is divided into several phases, which can be summarized as follows:
- anesthesia;
- access flap;
- bone resection;
- odontotomy;
- suture.
Each phase of the intervention has been studied to prevent the following possible complications:
- anesthesia: damage to facial nerve and parotid gland;
- access flap: damage to lingual nerve and periodontium of second molars;
- bone resection and odontotomy: damage to the periodontium of second molars, to mandibular alveolar and lingual nerves;
- suture: post-operative infection and periodontal damage to second molars.
In particular, odontotomy performed according to rational criteria is done to reduce excessive bone resection, extraction forces and necessity to carry the surgical instruments too deeply; therefore, a proper odontotomy plays a key role in reducing the most dangerous damages, especially those to the inferior alveolar nerve.
Anesthesia
The extraction of impacted and semi-impacted third molars is performed under local anesthesia in almost all cases.
The anesthetic of choice is articaine with adrenaline 1:100,000.
Anesthesia is performed in the following consecutive stages:
- troncular to the Spix’s spine;
- troncular to the buccal nerve;
- local, in the buccal fornix between the second and the third molar and on the external surface of the mandible;
- local, a limited amount in the retromolar region, on the lingual side as well.
Access flap
The incision of soft tissues has to be designed so as:
- to provide sufficient access;
- not to damage the surrounding anatomical structures, in particular the lingual nerve;
- to allow a correct and possibly easy suture.
The third molar is not strictly just behind the second molar, as it could be suspected from the OPG, but it is more often situated buccally, with the long axis directed medially.
This implies that the area immediately behind the second molar is likely crossed by the lingual nerve.
The flap is therefore obtained by means of two incisions: the first begins from the disto-lingual corner of the second molar and moves buccally and distally for about 15 mm with an angle of about 45°; the second begins from the first incision and continues forward in the gingival sulcus of the second molar, straight to its mesio-buccal corner.
The flap elevation is performed starting from the sulcus of the second molar and is completed with the incision of the periosteum.
The mucosal triangle bounded by the two incisions is removed to allow a better periodontal healing and drainage of the wound.
This approach delimits a triangular flap which allows an adequate surgical access and a stable divarication.
In case of semi-impaction, the first incision begins from the most distal point of the area of eruption of the third molar and continues buccally and distally for about 1 cm.
Bone resection and tooth dislocation
The goals of the bone resection are: exposure of at least half of the dental crown and creation of a buccal groove ensureing a favorable leverage point.
The dislocation is performed with angled levers of Friedman.
Odontotomy
Impacted and semi-impacted third molars cannot quite never be extracted entirely, because the trajectory of extraction could impact the second molar, the branch of the jaw or the lingual bone plate. Moreover, the roots of the third molar could be highly retentive.
Odontotomy is then used for:
- eliminate the crown portions which block the natural trajectory of extraction, without deleting gripping points useful for extracting the roots;
- separate the retained curved roots;
- save as much bone tissue as possible.
Tungsten carbide burs mounted on a high speed handpiece are used to fragment the tooth; such instrumentation allows to separate the tooth easily and very fast, although in the presence of a considerable thickness of enamel.
The high speed burs are very effective but require attention when they get closer to the surrounding structures: the inferior alveolar nerve, the lingual nerve, the second molar and the bone. The bur works safely until it is inside the tooth.
The odontotomy starts with a drill but always ends with a hand-made fracture by inserting a lever into the breach made by the bur itself.
The fragments of the crown can be swallowed or, even worse, aspirated in the airways. In order to prevent such an occurrence, they have to be firmly gripped, for example with a gripper for fragments. The smaller mobile fragments can be taken easily with the aspiration cannula.
The odontotomy is the cornerstone of any approach to surgical removal of mandibular third molars. When executed according to specific criteria, it reduces significantly the risk of damage. A careless and not well planned odontotomy is probably responsible for the high frequency of neurological damage also reported in some published studies.
Below a schematic animation useful to display the odontotomy phases of a horizontally impacted third molar is shown. Please note that the coronal fragment often requires further subdivision.
Animation by Tommaso Clauser
Suture
The goals of the suture are: hemostasis and tissues fixation in the best position.
The main difficulties encountered are usually related to the second molar. If a stitch is given match the flap margin to the lingual tissue, the flap could be lifted upwards; consequently, a pseudo-pocket behind the distal area of the second molar could be created.
To avoid these drawbacks, the suture must position the flap margin in correspondence of the dentin-enamel junction. This could be easily done with a mattress point, which anchors the flap behind the second molar as apically as possible. As a consequence, the fornix is not altered, the formation of a pseudo-pocket is prevented and the dental hygiene in the post-operative and healing period is facilitated.
The technique of the mattress suture is shown by means of a movie on a model, so as to to clarify each step.
The reported technique allows to place the flap in the original location or to a more apical and therefore more favorable site but does not completely close the wound, providing a favorable drainage.
Conclusions
A rational approach to the surgical removal of an impacted or semi-impacted mandibular third molar should first allow to prevent damage to the surrounding anatomical structures, such as the lingual nerve, the inferior alveolar nerve and the periodontium of the second molar.
The literature reports often high percentages of damage, both to inferior alveolar and lingual nerves, associated with obsolete and not well described surgical approaches, usually referred as “gold standard technique”.
The standard surgical technique is a myth to dispel, it does not exist.
The technique has evolved along with the technology: for example, the introduction of high speed handpieces designed for surgery (tilted to 135° and cooled without air) has made possible a much less invasive approach than that imposed by the traditional straight handpiece, which often obliged to demolish the buccal cortical bone.
Moreover, the advent of piezosurgery allows, nowadays, to work saely next to the alveolar canal.
Obviously, in addition to the technique, a clinician should always keep in mind the following points:
- the careful study of the clinical case is necessary to establish the risk/benefit ratio of the intervention: when the indication is clear, it is more reasonable to accept the risk;
- there is a close relationship between the post-extractive complications and the patient’s age: most of the current literature indicates a clear worsening of the prognosis after 25 years of age (Chiapasco et al, 1993; Cheung et al, 2010; Guidelines SIGN , 2000).
Therefore, the rational approach to the extraction of impacted and semi-impacted mandibular third molars can be summarized as follows:
- careful evaluation of the indications;
- choice the best time to operate;
- careful planning of the case;
- use of an adequate instrumentation;
- adoption of a minimally invasive technique.
REFERENCES
For further information about the role of patient’s age, local anatomy and expertise of operators in defining the risk of complications, see:
- Valmaseda-Castellón E, Berini-Aytés L, Gay-Escoda C. Inferior alveolar nerve damage after lower third molar surgical extraction: a prospective study of 1117 surgical extractions. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2001;92:377-83.
- Bui CH, Seldin EB, Dodson T. Types, frequencies, and risk factors for complications after third molar extraction. J Oral Maxillofac Surg 2003;61:1379-89.
- Queral-Godoy E. Valmaseda-Castellón E., L.Berini-Aytés,C. Gay-Escoda . Incidence and evolution of inferior alveolar nerve lesions following lower third molar extraction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2005;99:259-64.
- Haug, RH, Perrott DH, Gonzalez, Talwar RM. The American Association of Oral and Maxillofacial Surgeons Age-Related Third Molar Study. J Oral Maxillofac Surg 2005;63:1106-14.
- Chuang SK; Perrott DH, Susarla SM, Dodson TB. Age as a risk factor for third molar surgery complications. J Oral Maxillofac Surg 2007;65:1685-92.
- Cheung LK, Leung YY, Chow LK, Wong MC, Chan EK, Fok YH. Incidence of neurosensory deficits and recovery after lower third molar surgery: a prospective clinical study of 4338 cases. Int J Oral Maxillofac Surg 2010;39:320-6.
- Bruce RA, Frederickson GC, Small GS. Age of patients and morbidity associated with mandibular third molar surgery. J Am Dent Ass 1980;101:240-45.
- Chiapasco M, De Cicco L, Marrone G. Side effect complications associated with third molar surgery. Oral Surg Oral Med Oral Pathol 1993;76:412-20.
- Kunkel M, Kleis W, Morbach T, Wagner W. Severe third molar complications including death-lessons from 100 cases requiring hospitalization. J Oral Maxillofac Surg. 2007 Sep;65(9):1700-6.
- Kaminishi RM, Kaminishi KS. New considerations in the treatment of compromised third molars. J Calif Dent Ass 2004; 32(10): 823-5.
- Rood JP, Shehab BAA.The radiological prediction of inferior alveolar nerve injury during third molar surgery. Br J Oral Maxillofac Surg 1990;28:20-5.
- Jerjes W, Upile T, Shah P, Nhembre F, Gudka D, Kafas P, McCarthy E, Abbas S, Patel S, Hamdoon Z, Abiola J, Vourvakis M, Kalkani M, All-Khawalde M, Leerson R, Banu B, Rob J, El-Maaytah M, Hopper C. Risk factors associated with injury to the inferior alveolar and lingual nerves following third molar surgery-revisited. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2010;109:335-45.
For literature reviews, see:
- Scottish Intercollegiate Guidelines Network. Management of unerupted and impacted third molar teeth (Marzo 2000) http://www.sign.ac.uk/guidelines/fulltext/43/index.html. Consultato il 6-12-2011
- Mettes TG, Nienhuijs ME, van der Sanden WJ et al. Interventions for treating asymptomatic impacted wisdom teeth in adolescents and adults. Cochrane Database Syst Rev 2005; 18: 2.
For legal regulations about X-rays, see:
- Decreto Legislativo del 26 maggio 2000, n. 187. Attuazione della direttiva 97/43/Euratom in materia di protezione sanitaria delle persone contro i pericoli delle radiazioni ionizzanti connesse ad esposizioni mediche. Gazzetta Ufficiale n. 157 del 07-07-2000.
For further information about periodontal implications, see:
- Kugelberg CF. Impacted lower third molars and periodontal health. An epidemiological, methodological, retrospective and prospective clinical study. Swed Dent J 1990; 68(suppl): 1-52.
- Kugelberg CF, Ahlstrom U, Ericson S et al. Periodontal healing after lower third molar surgery in adolescents and adults. A prospective study. Int J Oral Maxillofac Surg 1991; 20(1): 18-24.
For further information about the role of third molars in (not) determining teeth crowding, see:
- Niedzielska I. Third molar influence on dental arch crowding. Eur J Orthod 2005; 27(5): 518-23.
- Zachrisson BU. Mandibular third molars and late lower arch crowding-the evidence base. World J Orthod 2005; 6(2): 180-6.
For further information about the consequences of the permanence of impacted or semi-impacted third molars, see:
- Guven O, Keskin A, Akal UK. The incidence of cystis and tumors around impacted third molars.Int J Oral Maxillofac Surg 2000; 29:13-5.
For further information:

